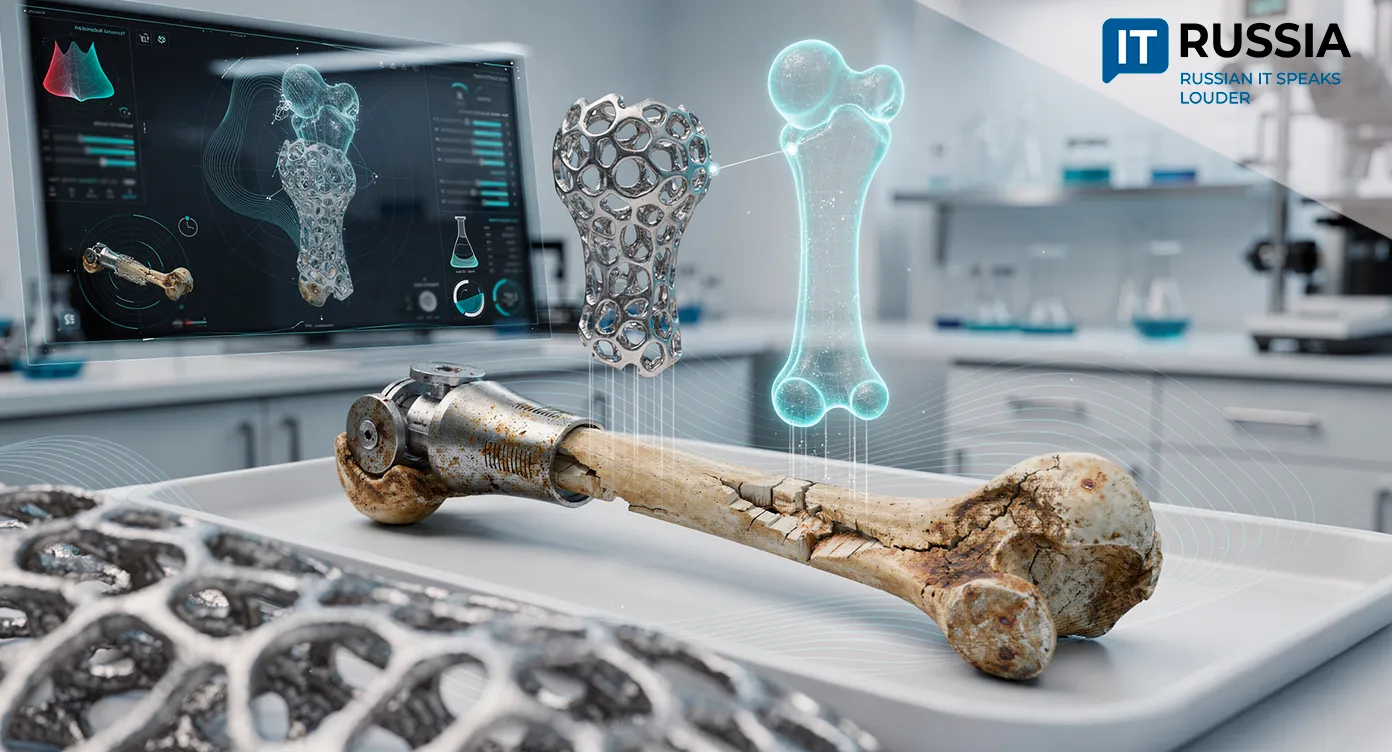
Russian and Iranian Scientists Are Building a 3D Tumor Model to Study Liver Cancer
Researchers at Sechenov University and Iran’s Royan Institute are developing a three-dimensional model of the liver tumor microenvironment to study hepatocellular carcinoma under a project supported by a Russian Science Foundation grant.

As healthcare systems become increasingly digitized and cancer treatment technologies continue to advance, personalized medicine is evolving rapidly. The field is built around the analysis of the molecular and genetic variability unique to each malignant tumor.
For years, anticancer drug development relied on the assumption that tumors with identical histopathology would respond to therapies in roughly the same way. Over time, however, researchers found that this framework overlooked the individual phenotypic and genotypic characteristics of both tumors and their surrounding microenvironments. In practice, that gap often resulted in lost time and worsening patient outcomes, including fatal cases. The transition from preclinical models to clinical trials has therefore become one of oncology’s most vulnerable stages. Selecting an adequate preclinical model is now considered one of the key factors shaping the outcome of cancer research.

Computer Vision Learns to Analyze Cancer Cell Behavior
Researchers at Sechenov University, working together with colleagues from Iran’s Royan Institute, will create a 3D tumor microenvironment model designed to replicate real tissue as closely as possible. Hepatocellular carcinoma is one of the most aggressive forms of liver cancer. It remains difficult to treat because of frequent relapses and strong resistance to therapy. Scientists link that resistance to stem-like cells, a small subpopulation capable of unlimited division and transformation into different types of tumor cells.
To study their behavior, researchers will create 3D organoids, miniature tumor models that reproduce both the structure and cellular diversity of living tissue. The project combines biophotonics, FLIM microscopy, small interfering RNA and artificial intelligence. Together, these systems make it possible to recreate conditions that closely resemble those inside a patient’s body. The central innovation lies in the fact that computer vision systems are now learning to analyze cancer cell behavior at the microscopic level. This is not simply a laboratory experiment. It represents a prototype for a future personalized medicine platform.

“Invisible” Cells Become Visible to Algorithms
The project’s core scientific objective is the study of stem-like tumor cells. These cells form a protective perimeter around tumors, enabling therapy resistance and triggering relapses. Traditional 2D cultures cannot reproduce the complex architecture of living tissue. By contrast, 3D organoids recreate cellular heterogeneity, spatial organization and elements of the tumor microenvironment, including fibroblasts. Researchers will use fluorescence lifetime imaging microscopy to analyze the models. Artificial intelligence has become the project’s main technological driver. Unlike algorithms trained to sort X-rays, these neural networks work with cellular imagery, calculating metabolic states and identifying the most therapy-resistant populations. The shift marks a transition from clinical radiology to digital biology.
The Evolution of Medical AI
Russia’s medical IT strategy is undergoing a broader transition. Five years ago, most attention focused on automating screening systems. Today, algorithms are moving into fundamental biomedical research. Earlier developments, including OncoPro and metastasis prediction systems introduced in 2025, laid the groundwork for that shift. The current project brings AI directly into the laboratory, where it acts as a research partner rather than simply an analytical tool. For Russian medicine, this creates a direct pathway toward implementing the Farma-2030 strategy. The combination of organoids, biophotonics and machine vision is forming a high-tech environment for preclinical testing. In the long term, patients could gain access to highly targeted therapy selection tools, while physicians may reduce the risk of prescribing ineffective treatment regimens.

Global Partnerships and the Export of Expertise
The collaboration with Iran, together with a newly signed memorandum with Shanghai Sixth People’s Hospital to create a mirror laboratory, points toward deeper cooperation with BRICS countries and Asian partners. Over the next several years, the focus is likely to shift toward exporting technologies, including software for cellular image analysis, validated organoid cultivation protocols and specialized scientific expertise. Russia’s work in personalized oncology is becoming an increasingly valuable asset in the global preclinical research market, giving the country an opportunity to participate in shaping future standards for biomedical data analysis.
Toward Cell-Level Treatment
In the near term, researchers expect scientific publications, validated protocols and a detailed map of the metabolic vulnerabilities of resistant cancer cells. Within three to five years, the technology could become an industry standard for testing new molecular compounds. Over a longer horizon, the system may move directly into clinical workflows. A patient’s biomaterial could be transformed into an individualized 3D clone, AI systems would analyze drug responses and oncologists would receive personalized treatment forecasts. Oncology is steadily moving toward a future in which therapies are selected not “by statistics,” but “by cell.” In that transition, Russia is positioning itself not as an observer, but as a contributor to the next generation of cancer medicine.